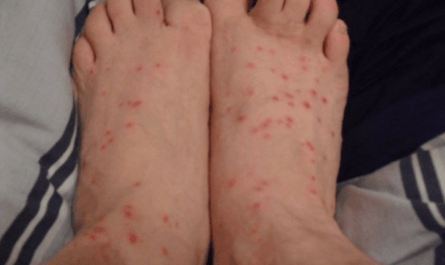
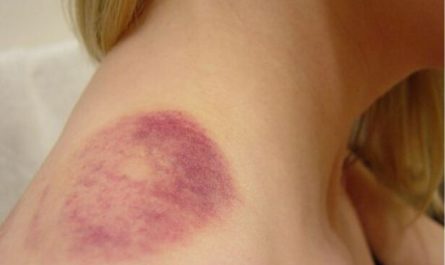
Yeast infection on the skin can be an uncomfortable and frustrating condition to deal with. It is caused by the overgrowth of a type of fungus called Candida, which is naturally present in the body. When the balance of bacteria and yeast in the body is disrupted, it can lead to an overgrowth of yeast and result in an infection.
While several over-the-counter and prescription medications are available to treat yeast infections, many people prefer natural remedies due to their effectiveness and minimal side effects. This article will explore the 12 best natural remedies for yeast infection on the skin.
What is a Yeast Infection?
A yeast infection, also known as candidiasis, is a common fungal infection that can occur in various body parts, including the skin. It is caused by an overgrowth of a type of yeast called Candida.
Candida is naturally present in the body, typically residing in areas like the mouth, gastrointestinal tract, and vaginal area without causing harm. However, certain factors can disrupt the natural balance of yeast, leading to overgrowth and subsequent infection.
Yeast infections on the skin, specifically, occur when Candida overgrows in the outer layers of the skin. This can result in symptoms such as itching, redness, inflammation, and a rash or patches on the affected area.
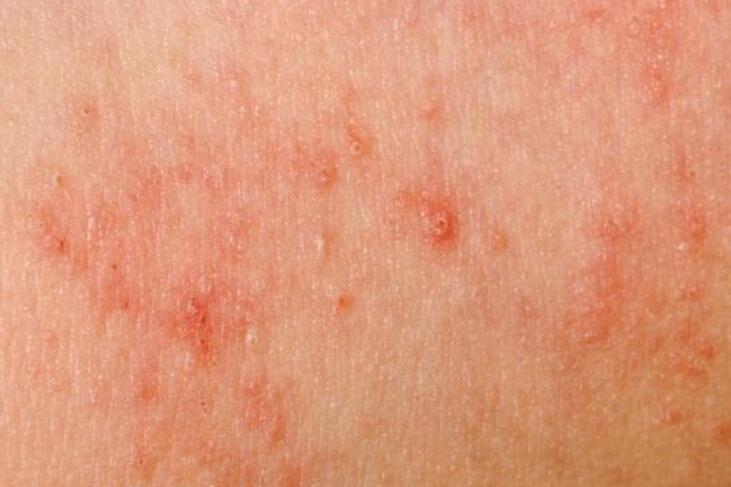
10 Common Causes of Yeast Infection on the Skin
Here are some common causes of yeast infections on the skin:
1. Warm and Moist Environment
One of the common causes of yeast infection on the skin is a warm and moist environment. Yeast thrives in such conditions, making areas of the skin with folds or excessive sweating more susceptible to infection. Common areas affected include the groin, armpits, and under the breasts.
2. Poor Hygiene Practices
Poor hygiene practices can also contribute to yeast infections on the skin. Failing to keep the skin clean and dry provides an ideal environment for yeast to multiply. Regularly washing and thoroughly drying the skin can help prevent yeast infections.
3. Weakened Immune System
A weakened immune system can make individuals more prone to yeast infections on the skin. Conditions like HIV/AIDS, diabetes, and prolonged use of immunosuppressant medications can compromise the immune system’s ability to keep yeast growth in check.
4. Antibiotic Use
The use of antibiotics is another common cause of yeast infections on the skin. Antibiotics target harmful bacteria and can disrupt the balance of yeast in the body, leading to overgrowth and subsequent infection. It is important to discuss with your healthcare provider about potential side effects and ways to mitigate the risk of yeast infections when taking antibiotics.
5. Hormonal Changes
Hormonal changes can play a role in developing yeast infections on the skin. Fluctuations in hormone levels, such as those experienced during pregnancy, can create an environment conducive to yeast overgrowth. Proper hygiene and regular monitoring can help manage yeast infections during these periods.
6. Tight Clothing
Wearing tight clothing, particularly in areas prone to sweating, can create an environment that promotes yeast growth. The lack of airflow and increased moisture retention provide an ideal breeding ground for yeast. Opting for loose-fitting clothing made from breathable fabrics can help prevent yeast infections.
7. Skin Injuries or Damages
Skin injuries or damages, such as cuts, scrapes, or burns, can allow the yeast to invade the skin and cause an infection. It is crucial to properly clean and care for any skin injuries to minimize the risk of yeast overgrowth.
8. Excessive Sugar Consumption
Excessive sugar consumption can contribute to yeast infections on the skin. Yeast feeds on sugar, and a high-sugar diet can fuel its growth. Limiting sugar intake, especially refined sugars, and processed foods, can help prevent yeast infections.
9. Certain Medications
Certain medications, such as corticosteroids and oral contraceptives, can disrupt the balance of yeast in the body and increase the risk of infection. If you take any medications affecting yeast levels, it is important to be vigilant and take necessary precautions to prevent yeast infections.
10. Weakened Skin Barrier
A weakened skin barrier can make the skin more susceptible to yeast infections. Factors compromising the skin barrier include excessive washing, harsh soaps or cleansers, and certain skin conditions like eczema or psoriasis.
Maintaining a healthy skin barrier through proper skin care practices can help reduce the risk of yeast infections.
12 Home Remedies for Yeast Infection on Skin
1. Tea Tree Oil
Tea tree oil is a powerful natural antifungal agent that can effectively combat yeast infections on the skin. It contains compounds called terpenes, which have antifungal properties and help inhibit the growth of Candida.
- Dilute a few drops of tea tree oil with a carrier oil, such as coconut oil.
- Apply the mixture to the affected area using a cotton ball or clean fingers.
- Leave it on for a few hours before rinsing it off.
- Repeat this process twice daily until the infection clears up.
2. Coconut Oil
Coconut oil is another excellent natural remedy for yeast infections on the skin. It contains lauric acid, which has antifungal properties and can help kill the Candida fungus.
- Take a small amount of coconut oil and warm it up to liquefy if necessary.
- Use clean fingers to apply a thin layer of coconut oil to the affected area.
- Leave it on for a few hours before rinsing it off.
- Repeat this process several times a day for optimal results.
3. Apple Cider Vinegar

Apple cider vinegar is a popular natural remedy for various health conditions, including yeast infections. It has antimicrobial properties that can help fight off the Candida fungus.
- Mix equal parts of apple cider vinegar and water.
- Apply the solution to the affected area using a cotton ball.
- Leave it on for a few minutes before rinsing it off.
- Repeat this process daily until the infection improves.
4. Garlic
Garlic is well-known for its antifungal and antibacterial properties, making it an effective natural remedy for yeast infections. It contains a compound called allicin, which exhibits potent antifungal activity.
- Peel and crush a few garlic cloves to create a paste.
- Apply the paste directly to the affected area.
- Leave it on for 30 minutes before rinsing it off with warm water.
- Repeat this process twice daily until the infection subsides.
5. Yogurt
Yogurt is a probiotic food that contains live cultures of beneficial bacteria, such as Lactobacillus acidophilus. These bacteria help restore the natural balance of microorganisms in the body and prevent the overgrowth of yeast.
- Take plain, unsweetened yogurt.
- Apply a generous amount of yogurt to the affected area.
- Leave it on for 30 minutes before rinsing it off.
- Repeat this process twice daily until the infection clears up.
6. Oregano Oil
Oregano oil is a potent natural antifungal agent that can effectively treat yeast infections on the skin. It contains compounds such as carvacrol and thymol, which have strong antifungal properties.
- Mix a few drops of oregano oil with carrier oil, such as coconut oil.
- Apply the mixture to the affected area using a cotton ball or clean fingers.
- Leave it on for a few hours before rinsing it off.
- Repeat this process daily until the infection improves.
7. Calendula
Calendula, also known as marigold, has anti-inflammatory and antifungal properties that make it beneficial for treating yeast infections on the skin. It can help reduce itching, redness, and inflammation associated with the infection.
- Take calendula cream or ointment.
- Apply a thin layer to the affected area two to three times a day.
- Gently massage it into the skin until fully absorbed.
- Repeat this process until the infection subsides.
8. Aloe Vera

Aloe vera has soothing and healing properties that can relieve the discomfort caused by yeast infections. It can help reduce inflammation and promote skin healing.
- Cut open an aloe vera leaf and extract fresh gel from it.
- Apply the gel directly to the affected area.
- Leave it on for 20-30 minutes before rinsing it off.
- Repeat this process two to three times a day until the infection clears up.
9. Boric Acid
Boric acid is a natural antiseptic that can be used to treat yeast infections on the skin. It has antifungal properties and helps restore the pH balance of the affected area, creating an unfavorable environment for yeast growth.
- Dissolve a teaspoon of boric acid in a cup of water.
- Apply the solution to the affected area using a cotton ball.
- Leave it on for a few minutes before rinsing it off.
- Repeat this process once or twice daily until the infection improves.
10. Cranberry Juice
Cranberry juice can not only help prevent urinary tract infections but can also be beneficial for yeast infections on the skin. Cranberries contain compounds that help inhibit yeast growth and prevent it from adhering to the skin.
- Drink unsweetened cranberry juice daily.
- Apply unsweetened cranberry juice topically to the affected area.
- Leave it on for a few minutes before rinsing it off.
- Repeat this process for best results.
11. Grapefruit Seed Extract
Grapefruit seed extract is a natural antimicrobial agent that can effectively fight yeast infections on the skin. It contains compounds such as polyphenols and limonoids, which have antifungal properties.
- Mix a few drops of grapefruit seed extract with a carrier oil.
- Apply the mixture to the affected area using a cotton ball or clean fingers.
- Leave it on for a few hours before rinsing it off.
- Repeat this process twice daily until the infection subsides.
12. Probiotics
Probiotics are beneficial bacteria that can help restore the natural balance of microorganisms in the body and prevent yeast overgrowth.
- Take a high-quality probiotic supplement daily or consume probiotic-rich foods.
- Follow the recommended dosage instructions for the supplement.
- Consume probiotic-rich foods such as yogurt, kefir, and sauerkraut regularly.
FAQs
1. Are yeast infections contagious?
Yeast infections are not contagious traditionally and cannot be spread through casual contact. However, a partner can develop a yeast infection through sexual activity if yeast is overgrowth.
2. Can over-the-counter antifungal creams treat yeast infections on the skin?
Over-the-counter antifungal creams can effectively treat mild yeast infections on the skin. However, if the infection persists or worsens, it is important to consult a healthcare professional for further evaluation and treatment.
3. How long does it take for natural remedies to work on yeast infections?
The time it takes for natural remedies to work on yeast infections can vary depending on the severity of the infection and the individual’s response to the treatment. In most cases, consistent use of natural remedies for a few weeks can lead to significant improvement.
4. Can men get yeast infections on the skin?
Yes, men can also develop yeast infections on the skin, especially in areas such as the groin, armpits, and under the breasts. The same natural remedies mentioned in this article can be used to treat yeast infections in men.
5. Are there any preventive measures for yeast infections on the skin?
Maintaining good hygiene practices, keeping the skin clean and dry, avoiding tight-fitting clothing, and limiting sugar intake are some preventive measures that can help reduce the risk of yeast infections on the skin.
6. When should I see a doctor?
If the yeast infection does not improve after several weeks of using natural remedies or if the symptoms worsen, it’s recommended to consult a healthcare professional. They can provide a proper diagnosis and suggest appropriate treatment options.